January 22, 2016. Today started out well. I started to work at 3:45 A.M. and stopped about three hours later for a breakfast break. I was surprised to learn that Dad was still sleeping. A few minutes after I returned to work, I heard Dad and Dianne talking in the bedroom. After she unplugged him from the tube feed, he used the walker to go into the closet to pick out his clothes for the day, and then he got dressed. Dianne later told me that it was a blessing to witness how far he had come.
 Dad, Dianne, and Mom ate breakfast at 8:15 A.M., Dad having his usual Cream of Wheat with honey, and a pear. About 90 minutes later, he said that he didn’t feel well, and then started vomiting. Surprisingly, he vomited only mucus and not his breakfast. I was perplexed about what might have caused the vomiting. Fortunately, Stephanie, the nurse, had already called us and was scheduled to arrive within the hour.
Dad, Dianne, and Mom ate breakfast at 8:15 A.M., Dad having his usual Cream of Wheat with honey, and a pear. About 90 minutes later, he said that he didn’t feel well, and then started vomiting. Surprisingly, he vomited only mucus and not his breakfast. I was perplexed about what might have caused the vomiting. Fortunately, Stephanie, the nurse, had already called us and was scheduled to arrive within the hour.
When Stephanie arrived, she couldn’t shed any light on why he might have been sick. She said that although he seemed to have a lot of phlegm, his lungs sounded clear. She and I then had a long talk about the amount of fluid that was being removed from him during dialysis. He didn’t appear to be retaining any fluid, and his dry weight seemed low to me. Stephanie was no nephrologist, but I asked her if she thought that measuring Dad’s ankles every day might help us to determine his level of fluid retention. She said that she thought that that was a good idea and suggested that we give it a try.
Janet stopped by for Dad’s occupational therapy session, and she and Dad had a long discussion about his lack of exercise between their sessions. He didn’t like to do it, and I doubted that anything she said would make any difference. She said that she would return next week, but I didn’t know how much more we’d see of her after that. She had been working with Dad on building up his core, and today I was pleased when I learned that she would lead both Mom and Dad through the exercises. I had Dianne record the session so that they could repeat the exercises when Janet wasn’t here.
 When Janet left, I took a break from work to eat lunch. When I returned to my computer about an hour later, I was greeted by the blue screen of death. I called my employer’s help desk and ran through some diagnostic tests to determine if we could fix the problem, but the tech finally said that he would open an urgent issue. I was lucky. The now-dead computer was very new, and I still had my old laptop with me. The IT tech from the Houston office called me and said that he was sending me a loaner computer via FedEx, which meant that I wouldn’t need to drive 60 miles to our Austin office, which had been a concern. I spent the remainder of my workday using my old computer to work on a website. I was thankful that I had enabled daily backups of my computer.
When Janet left, I took a break from work to eat lunch. When I returned to my computer about an hour later, I was greeted by the blue screen of death. I called my employer’s help desk and ran through some diagnostic tests to determine if we could fix the problem, but the tech finally said that he would open an urgent issue. I was lucky. The now-dead computer was very new, and I still had my old laptop with me. The IT tech from the Houston office called me and said that he was sending me a loaner computer via FedEx, which meant that I wouldn’t need to drive 60 miles to our Austin office, which had been a concern. I spent the remainder of my workday using my old computer to work on a website. I was thankful that I had enabled daily backups of my computer.
While I was playing with blue screens and the help desk, Dianne and Dad were walking around the house and running through his balancing routines at the laundry room sink. During happy hour, he navigated himself into the sunken sunroom. He still needed some assistance to step out of the room, but his skill with the walker was improving.
 We were finished with our dinner of enchiladas and chocolate cake before 7:00 P.M. Dianne was getting better at Oh Hell and was tonight’s winner. We were finished with our card game by 7:30 P.M., and by 7:55 P.M. Dad was drifting off to sleep.
We were finished with our dinner of enchiladas and chocolate cake before 7:00 P.M. Dianne was getting better at Oh Hell and was tonight’s winner. We were finished with our card game by 7:30 P.M., and by 7:55 P.M. Dad was drifting off to sleep.
January 23. Although it was Saturday morning, I woke up shortly after 3:00 A.M. While I was lying in bed wondering why I was awake, I heard a loud crash through the baby monitor. I jumped out of bed and ran downstairs and into Dad’s room. It seemed that he had swung he feet out of bed and was attempting to get out of bed, forgetting that he was attached to the tube feed, which hung on an IV pole. Having the contraption fall was only a small problem. The fact that Dianne had not secured the top of the tube-feed bag when she refilled it was quite another. The sticky Nepro seemed to have been sprayed all over Dad, his bed, and the floor. Once again, I was very thankful that Stan had purchased floor mats to cover my parents’ bedroom carpeting.
While Dianne was cleaning up after Dad’s handiwork, Dad wheeled himself into the bathroom and got himself cleaned up for breakfast. After his breakfast of Cream of Wheat, he wanted another cup of hot water, which prompted another knock-down drag-out about what he could and could not do with water. Kristen, the speech therapist, had told him on numerous occasions that he could not drink water unless his mouth was clean. Drinking water immediately after eating was strictly forbidden—at least for now. I reminded him that by March 1st I would be out of here, even if he gave himself pneumonia again by aspirating on food particles.
 Mom and I were still concerned about Dad’s dry weight and followed his bus to the dialysis center so that we could talk with his nurse about the amount of fluid they had been removing. We had spoken with Sue, our friend and nurse practitioner, only a week ago, but I still thought that they were removing too much. After speaking with the charge nurse, she said that they would remove only the minimal amount—1200 ml. Mom and I had been loaded for bear, and the encounter with the nurse was very anticlimactic.
Mom and I were still concerned about Dad’s dry weight and followed his bus to the dialysis center so that we could talk with his nurse about the amount of fluid they had been removing. We had spoken with Sue, our friend and nurse practitioner, only a week ago, but I still thought that they were removing too much. After speaking with the charge nurse, she said that they would remove only the minimal amount—1200 ml. Mom and I had been loaded for bear, and the encounter with the nurse was very anticlimactic.
On the way home from the dialysis center, Mom and I stopped at HEB. I preferred shopping during early morning hours when no one was around except the people who restocked the shelves. When we pulled into the parking lot, we noticed the strangest sight—hundreds of blackbirds were sleeping in the parking lot. Dozens of them were on the ground, and many others were sitting on the tops of the employees’ cars. As we drove through the parking lot, they didn’t stir. They remained still as we walked passed them and into the store. By the time that we left the store, the birds were gone.
Stan arrived from Houston at noon. He hadn’t been in the house for more than two minutes where we heard the HOP bus arrive with Dad and Dianne. Dianne reported that Dad had weighed in at 66.2 kg, and true to her word, the nurse had removed only 1190 ml of fluid, leaving Dad weighing 65.4 kg.
 After lunch, Mom and I ran a couple of errands, and when we returned, Stan and Dad were playing cribbage. After beating Stan at a couple of games, Dad finally wanted to take a nap. He told Dianne that he wanted to get up by 5:00 P.M., a little less than two hours from now. She tried to wake him at 4:45 P.M. and then again 45 minutes later. She was finally able to rouse him at 5:50 P.M., but he stated that he didn’t feel right. He joined us in the living room as we were ending our happy hour. Dianne prepared some shaved ice for him, and during the remainder of our happy hour, Dad talked a lot about his mother and her final days battling Guillan Barre Syndrome.
After lunch, Mom and I ran a couple of errands, and when we returned, Stan and Dad were playing cribbage. After beating Stan at a couple of games, Dad finally wanted to take a nap. He told Dianne that he wanted to get up by 5:00 P.M., a little less than two hours from now. She tried to wake him at 4:45 P.M. and then again 45 minutes later. She was finally able to rouse him at 5:50 P.M., but he stated that he didn’t feel right. He joined us in the living room as we were ending our happy hour. Dianne prepared some shaved ice for him, and during the remainder of our happy hour, Dad talked a lot about his mother and her final days battling Guillan Barre Syndrome.
We had a nice dinner, but Dad didn’t eat much. At Dad’s request, we played a longer game of Oh Hell and didn’t start heading toward bed until 8:45 P.M. After Dad got into bed, Dianne left the room to get ready for bed. She was gone for only a couple of minutes when Dad started complaining about not feeling well and about having the G-tube. As I was administering his meds into the G-tube, he started vomiting, and this time he was vomiting a lot more than mucus.
By the time that Dianne returned, Dad said that he was feeling better. To ensure that his night was less eventful, I also administered some Zofran into his G-tube. He seemed to be coughing a lot, so we had him move up in the bed, and I raised his head and feet. By 9:30 P.M., he seemed better and ready to go to sleep. I was certainly good and ready to go to bed.
January 24. I got up shortly before 6:30 A.M. and went downstairs to see Dad. I had heard through the monitor that he and Dianne were awake and he was asking her if he was tied up (his reference to being attached to the tube feed). He was feeling good, but he was somewhat grumpy and a little sarcastic. While he and I were exchanging barbs, Dianne left the room to take a shower and get dressed. When she returned, I went to my home office to see if I could make any progress with my loaner PC, which had arrived yesterday from my Houston office.
 We all had a nice breakfast together. Mom fixed scrambled eggs, sausage, and English muffins, and Dad had a little of each. While Mom and I attended church, Stan and Dad played cribbage. After lunch, Stan and Dad went out to the garden. They spent about 30 minutes outside and then sat on the patio for about 20 minutes, just enjoying the beautiful weather and each other’s company. Stan was Dad’s welcome relief from being surrounded by a bunch of women who seemed to do nothing but tell him what he could and could not do. By the time that the guys came indoors, it was after 3:00 P.M. and time for Stan to return to Houston.
We all had a nice breakfast together. Mom fixed scrambled eggs, sausage, and English muffins, and Dad had a little of each. While Mom and I attended church, Stan and Dad played cribbage. After lunch, Stan and Dad went out to the garden. They spent about 30 minutes outside and then sat on the patio for about 20 minutes, just enjoying the beautiful weather and each other’s company. Stan was Dad’s welcome relief from being surrounded by a bunch of women who seemed to do nothing but tell him what he could and could not do. By the time that the guys came indoors, it was after 3:00 P.M. and time for Stan to return to Houston.
After Stan left, the four of us watched the Denver Broncos beat the New England Patriots. My parents were diehard fans of the Denver Broncos and were thrilled at their victory over the Patriots. We monitored the game between the Carolina Panthers and Phoenix Cardinals during dinner and our game of Oh Hell. Dianne was a fan of the Panthers, so everyone in the house seemed pleased with the outcomes of the sporting events.
 We wrapped up our game of Oh Hell by 8:30 P.M., and by 9:15 P.M., all of were ready for bed. Before drifting off to sleep, I called Stan. He had texted me when he arrived home, but I needed to speak with him every night before I went to sleep.
We wrapped up our game of Oh Hell by 8:30 P.M., and by 9:15 P.M., all of were ready for bed. Before drifting off to sleep, I called Stan. He had texted me when he arrived home, but I needed to speak with him every night before I went to sleep.
January 25. I was up by 3:30 A.M. and at work with a cup of hot coffee within 15 minutes. The house was very quiet for the next 2-1/2 hours. I kept the office door closed, but by 6:00 A.M., I heard some sounds coming from Dad’s room. Dianne unhooked him from the tube feed, and Dad got up and got dressed for the day. He wheeled himself into the kitchen and prepared himself a cup of hot water while Mom prepared his Cream of Wheat and ½ pear for breakfast.
 While I was working, Dad and Dianne walked around the backyard for about an hour, which gave his legs a good workout.
While I was working, Dad and Dianne walked around the backyard for about an hour, which gave his legs a good workout.
Brenda arrived around 11:30 A.M. for Dad’s physical therapy session, and she concentrated on his balance, which would be important when he started walking with a cane.
Kristen arrived at 2:00 P.M. for Dad’s swallow therapy session. During this visit, she had Mom prepare a cup of hot coffee for Dad and had him take some sips of it. Once an avid coffee drinker, he now was not very enamored with the taste of coffee. It’s amazing how not eating for a few months can affect your taste buds. Kristen said that as long as he had a clean mouth and remembered to tuck his chin when he swallowed, she felt good about him drinking coffee. She added that on her next visit they would have thin liquids and a snack. Kristen left after only 30 minutes, at which time Dad decided to take a short nap.
In addition to Dad’s normal Monday activities and appointments, today was recertification and assessment day for Dad’s therapies. At 3:00 P.M., Kathleen arrived with Pam, the physical therapy shower aide, in tow. Kathleen reviewed Dad’s balance, walking with the walker, and his ability to transfer into and out of the car. She also had Pam work with me to ensure that I could properly apply the dressing to Dad’s port before he showered. Our aides were both trained, but their time with us was coming to a close, and Mom and I also needed this training. At the end of her time with us, Kathleen certified Dad for another 30 days of occupational and physical therapy. She said that he had great balance and that she would like to see Dad walking independently with a cane at the end of 30 days.
 After Kathleen and Pam left, I returned to work until happy hour, and Dad took a nap. After dinner and happy hour, Mom beat us at Oh Hell. It was an early evening, and Dad was in bed by 8:00 P.M. I couldn’t wait to call Stan and give him the good news about today’s events.
After Kathleen and Pam left, I returned to work until happy hour, and Dad took a nap. After dinner and happy hour, Mom beat us at Oh Hell. It was an early evening, and Dad was in bed by 8:00 P.M. I couldn’t wait to call Stan and give him the good news about today’s events.



 While I was finding my first cup of coffee, Dianne tried to interest Dad in a sponge bath, but he wouldn’t entertain the idea. During recent physical therapy sessions, he had practiced transitioning in and out of the shower, and he would have a “proper” shower after the holidays. Unfortunately, while he was holding out for a proper shower, he was accumulating several layers of dead skin, which caused flakiness and bumps to appear on his extremities. When I returned to his room to see how he was feeling, he said that he felt better than yesterday, but he wavered a bit when I helped him transition to his wheelchair.
While I was finding my first cup of coffee, Dianne tried to interest Dad in a sponge bath, but he wouldn’t entertain the idea. During recent physical therapy sessions, he had practiced transitioning in and out of the shower, and he would have a “proper” shower after the holidays. Unfortunately, while he was holding out for a proper shower, he was accumulating several layers of dead skin, which caused flakiness and bumps to appear on his extremities. When I returned to his room to see how he was feeling, he said that he felt better than yesterday, but he wavered a bit when I helped him transition to his wheelchair. After we all opened our presents, Mom, Stan, Dianne, and I enjoyed our family’s traditional breakfast of Christmas morning loaf and bear claws. After tidying the kitchen somewhat, I accompanied Dad as he wheeled himself from the bedroom to the sunken sunroom where we had the tree. Stan and Dianne helped Dad step down into the sunroom and over to a chair—a real chair and not the wheelchair. My parents and husband had long since resigned themselves to my insistence on our traditional family photo session on Christmas Day, but no one seemed to mind it this year. I usually came armed with fancy hats or other props, but this year I was just happy that our Christmas photo included the four of us.
After we all opened our presents, Mom, Stan, Dianne, and I enjoyed our family’s traditional breakfast of Christmas morning loaf and bear claws. After tidying the kitchen somewhat, I accompanied Dad as he wheeled himself from the bedroom to the sunken sunroom where we had the tree. Stan and Dianne helped Dad step down into the sunroom and over to a chair—a real chair and not the wheelchair. My parents and husband had long since resigned themselves to my insistence on our traditional family photo session on Christmas Day, but no one seemed to mind it this year. I usually came armed with fancy hats or other props, but this year I was just happy that our Christmas photo included the four of us. After Dad woke up, he and Stan played several hands of cribbage, and Stan finally won, which was a major feat as Dad was darn good at the game. Dad was still fighting a chest cold and Stan was fighting a migraine, so they were both ready for naps when they finished their grueling match. Mom and I didn’t want to take naps, but we eventually fell asleep while sitting on the couch.
After Dad woke up, he and Stan played several hands of cribbage, and Stan finally won, which was a major feat as Dad was darn good at the game. Dad was still fighting a chest cold and Stan was fighting a migraine, so they were both ready for naps when they finished their grueling match. Mom and I didn’t want to take naps, but we eventually fell asleep while sitting on the couch.

 When we arrived at the doctor’s office, the nurses and doctor were agog about Dad, repeating how much better he looked than he had just a few weeks earlier. The nurse said that seeing him “just made her day.” They were also pleased that he had gained a couple of pounds. His weight was up to 139 pounds. The dietitian said that if he passed his
When we arrived at the doctor’s office, the nurses and doctor were agog about Dad, repeating how much better he looked than he had just a few weeks earlier. The nurse said that seeing him “just made her day.” They were also pleased that he had gained a couple of pounds. His weight was up to 139 pounds. The dietitian said that if he passed his  Today, I drove 65 miles to Austin to attend an annual lunch with a group of former coworkers. It was a long way to go for lunch, but we had been meeting for about 15 years, and I always looked forward to seeing these guys. The luncheon also gave me an opportunity to share more of my holiday biscotti and experience one of my normal activities and traditions.
Today, I drove 65 miles to Austin to attend an annual lunch with a group of former coworkers. It was a long way to go for lunch, but we had been meeting for about 15 years, and I always looked forward to seeing these guys. The luncheon also gave me an opportunity to share more of my holiday biscotti and experience one of my normal activities and traditions. Today, however, was different. Although the paper was in the right place, Mom saw something on the front porch that kept her from opening the door. When Mom looked out of the front windows, she saw a large snake on the front porch, which wasn’t all that unusual. It scared her enough, though, that she wouldn’t open the door to get the paper, and she came to the office to get me—the biggest wuss in the world when it comes to snakes. When I looked out the front window, I had to laugh. The snake turned out to be a bungee cord that fell off of Timothy’s hand truck during his delivery last night. With the bravado of Crocodile Dundee’s better half, I boldly walked outside, captured the bungee snake, and picked up the newspaper.
Today, however, was different. Although the paper was in the right place, Mom saw something on the front porch that kept her from opening the door. When Mom looked out of the front windows, she saw a large snake on the front porch, which wasn’t all that unusual. It scared her enough, though, that she wouldn’t open the door to get the paper, and she came to the office to get me—the biggest wuss in the world when it comes to snakes. When I looked out the front window, I had to laugh. The snake turned out to be a bungee cord that fell off of Timothy’s hand truck during his delivery last night. With the bravado of Crocodile Dundee’s better half, I boldly walked outside, captured the bungee snake, and picked up the newspaper.
 The parade of provider assessments started with Kathleen, the physical therapist, at 10:30 A.M. She was followed at 11:30 A.M. by Janet, the occupational therapist, and at 1:30 P.M. by Stephanie, the nurse. During Kathleen’s visit, she asked how Dad was being transported to dialysis. We told her that we had wanted to use the
The parade of provider assessments started with Kathleen, the physical therapist, at 10:30 A.M. She was followed at 11:30 A.M. by Janet, the occupational therapist, and at 1:30 P.M. by Stephanie, the nurse. During Kathleen’s visit, she asked how Dad was being transported to dialysis. We told her that we had wanted to use the  Shortly after Mike left, Dad was ready for a nap, and he slept until it was time for him to swallow some ice chips. As he wheeled himself from his room, he stopped by the office to let me know that I should stop for the day because it was time for happy hour.
Shortly after Mike left, Dad was ready for a nap, and he slept until it was time for him to swallow some ice chips. As he wheeled himself from his room, he stopped by the office to let me know that I should stop for the day because it was time for happy hour. Gale had barely pulled out of the driveway when Brenda arrived for Dad’s physical therapy session. Brenda put him through his paces, having him walk 68 feet, march in place, stand on one foot, and stand on his toes. Dad was exhausted when she left and was ready for a nap. However, instead of sleeping until he woke up himself, he instructed Michell to wake him by 2:00 P.M.
Gale had barely pulled out of the driveway when Brenda arrived for Dad’s physical therapy session. Brenda put him through his paces, having him walk 68 feet, march in place, stand on one foot, and stand on his toes. Dad was exhausted when she left and was ready for a nap. However, instead of sleeping until he woke up himself, he instructed Michell to wake him by 2:00 P.M.
 When Michell and Dad were picked up by the EMS wheelchair van service, Stan and I drove to the dialysis center. I had been very upset that they had removed 2,500 ml from Dad on Thursday, and I intended to express my concern to the charge nurse. For each 1,000 ml removed, a dialysis patient loses 1 kg. After I had explained Dad’s situation, she said that they would just clean his blood today and not remove any fluid from him.
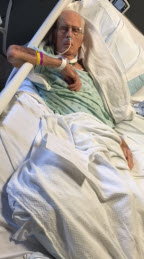
When Michell and Dad were picked up by the EMS wheelchair van service, Stan and I drove to the dialysis center. I had been very upset that they had removed 2,500 ml from Dad on Thursday, and I intended to express my concern to the charge nurse. For each 1,000 ml removed, a dialysis patient loses 1 kg. After I had explained Dad’s situation, she said that they would just clean his blood today and not remove any fluid from him. After I saw Dad weighed, Stan and I left Dad and Michell at the dialysis center so that we could run several errands before Dad returned home. Everything worked in our favor, and we were home by 10:30 A.M. As it turned out, Stan and I didn’t have to rush. Dad and Michell had to wait for the van and didn’t return home until after noon.
After I saw Dad weighed, Stan and I left Dad and Michell at the dialysis center so that we could run several errands before Dad returned home. Everything worked in our favor, and we were home by 10:30 A.M. As it turned out, Stan and I didn’t have to rush. Dad and Michell had to wait for the van and didn’t return home until after noon. Shortly before 2:00 P.M., Dad took a long nap on the couch while we were in the living room because he didn’t want to be away from us. I think that he thought that sleeping on the couch would ensure that he didn’t miss happy hour, but he slept through it. Dozing on the couch might not seem like a big deal, but it was another first for him in his post-hospital life. We had to rely on the oxygen tank and trach bib because we couldn’t bring the oxygen concentrator and nebulizer to the living room, but he was able to receive Nepro during his nap. He slept for about four hours, and we woke him when we finished dinner.
Shortly before 2:00 P.M., Dad took a long nap on the couch while we were in the living room because he didn’t want to be away from us. I think that he thought that sleeping on the couch would ensure that he didn’t miss happy hour, but he slept through it. Dozing on the couch might not seem like a big deal, but it was another first for him in his post-hospital life. We had to rely on the oxygen tank and trach bib because we couldn’t bring the oxygen concentrator and nebulizer to the living room, but he was able to receive Nepro during his nap. He slept for about four hours, and we woke him when we finished dinner. At 10:30 P.M., the baby monitor station in our room started alarming. After quickly putting on my glasses, I could read the message on the display that indicated that our station was unlinked from the base station. As I tried to turn on the light, I discovered that the
At 10:30 P.M., the baby monitor station in our room started alarming. After quickly putting on my glasses, I could read the message on the display that indicated that our station was unlinked from the base station. As I tried to turn on the light, I discovered that the  By 8:00 A.M., Dad was back in the wheelchair and was reading the Sunday newspaper. When Mom and I left for church, he and Stan were playing cribbage. After a couple of games of cribbage, Dad wanted to lie down and rest. According to Michell, he fell asleep as soon as his head hit the pillow. Usually, he liked for us to wake him before Stan left for Houston, but today he asked that we let him sleep.
By 8:00 A.M., Dad was back in the wheelchair and was reading the Sunday newspaper. When Mom and I left for church, he and Stan were playing cribbage. After a couple of games of cribbage, Dad wanted to lie down and rest. According to Michell, he fell asleep as soon as his head hit the pillow. Usually, he liked for us to wake him before Stan left for Houston, but today he asked that we let him sleep. November 23. Dad was very slow in waking up this morning. When I heard him and Michell talking, I took a break from work to administer his morning meds and trach care. Tracy, one of our RNs, called around 9:00 A.M.to see if we could be her first stop this morning. I was very low on the Mepilex dressings that American HomePatient didn’t provide and asked Tracy if she could bring me a few to tide me over until I could order more from Amazon. She said that she would stop by the office and pick up a couple for me. I was very fond of Tracy. She was a wonderful nurse and the mother of a special needs child. She was one of my favorite nurses and a very caring person. She arrived at my parents’ home at 10:00 A.M. with my requested dressing in hand. After her brief examination of Dad, she said that his bed sore was practically healed. With the way that Dad had been feeling, I didn’t want to take him back to the wound care doctor, which would most likely take the entire afternoon. She said that I could safely cancel his appointment with wound care today. Also, she didn’t think that I would need any more of the expensive Mepilex dressings. I happily accepted the good news and canceled the appointment with the doctor and the EMS wheelchair van service.
November 23. Dad was very slow in waking up this morning. When I heard him and Michell talking, I took a break from work to administer his morning meds and trach care. Tracy, one of our RNs, called around 9:00 A.M.to see if we could be her first stop this morning. I was very low on the Mepilex dressings that American HomePatient didn’t provide and asked Tracy if she could bring me a few to tide me over until I could order more from Amazon. She said that she would stop by the office and pick up a couple for me. I was very fond of Tracy. She was a wonderful nurse and the mother of a special needs child. She was one of my favorite nurses and a very caring person. She arrived at my parents’ home at 10:00 A.M. with my requested dressing in hand. After her brief examination of Dad, she said that his bed sore was practically healed. With the way that Dad had been feeling, I didn’t want to take him back to the wound care doctor, which would most likely take the entire afternoon. She said that I could safely cancel his appointment with wound care today. Also, she didn’t think that I would need any more of the expensive Mepilex dressings. I happily accepted the good news and canceled the appointment with the doctor and the EMS wheelchair van service. While Tracy was visiting, Dad spent the entire time either sitting or lying on the bed, so she didn’t see how weak he had become. Shortly before Tracy arrived, Michell had had to hold up Dad to keep him from falling when he was trying to get dressed. I hoped that we would hear something soon from Dr. Pfanner’s office.
While Tracy was visiting, Dad spent the entire time either sitting or lying on the bed, so she didn’t see how weak he had become. Shortly before Tracy arrived, Michell had had to hold up Dad to keep him from falling when he was trying to get dressed. I hoped that we would hear something soon from Dr. Pfanner’s office.

 November 11. Dad had another good night. I might have heard him cough twice. At 7:45 A.M., I was between meetings and wanted to administer trach care and meds, but Dad was still in bed and didn’t want to get up. I told him that he was a lazy bones and that we’d have to make “
November 11. Dad had another good night. I might have heard him cough twice. At 7:45 A.M., I was between meetings and wanted to administer trach care and meds, but Dad was still in bed and didn’t want to get up. I told him that he was a lazy bones and that we’d have to make “ Before Stephanie’s car left the driveway, Brenda pulled up behind her for Dad’s physical therapy session. I didn’t watch the session, but from what I could hear, it seemed like she was working with him on transfers. I once heard her say that Dad got an A on something that he did, but not an A+. At the end of the session, she said that he got a gold star for the day. I had to laugh to myself as I wondered about the type of psychology that they employed to get him to cooperate. On her way out, Brenda stopped by my office and asked me about the rubber mat for the shower that I had agreed to get during our discussion on
Before Stephanie’s car left the driveway, Brenda pulled up behind her for Dad’s physical therapy session. I didn’t watch the session, but from what I could hear, it seemed like she was working with him on transfers. I once heard her say that Dad got an A on something that he did, but not an A+. At the end of the session, she said that he got a gold star for the day. I had to laugh to myself as I wondered about the type of psychology that they employed to get him to cooperate. On her way out, Brenda stopped by my office and asked me about the rubber mat for the shower that I had agreed to get during our discussion on  November 12. Shortly before 3:30 A.M., I heard Dad call for Gale to help him to find the urinal. I got up shortly after that and woke them. I watched as Gale handled all of the meds and routine trach care this morning—her last practice run before I left for Houston. Everything ran smoothly, and we were ready when the wheelchair van arrived at 5:50 A.M., some 20 minutes early.
November 12. Shortly before 3:30 A.M., I heard Dad call for Gale to help him to find the urinal. I got up shortly after that and woke them. I watched as Gale handled all of the meds and routine trach care this morning—her last practice run before I left for Houston. Everything ran smoothly, and we were ready when the wheelchair van arrived at 5:50 A.M., some 20 minutes early. Gale had her first solo run with the meds and trach care right after I left. Dad took a nap until 3:00 P.M. and was up for the remainder of the day. The three of them played cards, and Mom won again. Gale got Dad in bed by 8:00 P.M. and had no problem administering his night time meds and trach care.
Gale had her first solo run with the meds and trach care right after I left. Dad took a nap until 3:00 P.M. and was up for the remainder of the day. The three of them played cards, and Mom won again. Gale got Dad in bed by 8:00 P.M. and had no problem administering his night time meds and trach care. Stephanie, the nurse, came by around noon to take Dad’s vitals and check his bedsore. She said that the bedsore was healing nicely and that it was looking great. Bless her heart; Stephanie also brought us enough trach lubricant to last for a couple of months. These home care nurses were wonderful. In hindsight, I don’t know if I ever told them how much I appreciated them.
Stephanie, the nurse, came by around noon to take Dad’s vitals and check his bedsore. She said that the bedsore was healing nicely and that it was looking great. Bless her heart; Stephanie also brought us enough trach lubricant to last for a couple of months. These home care nurses were wonderful. In hindsight, I don’t know if I ever told them how much I appreciated them.
 Later in the morning, I received a call from Barbara at the Scott & White gastroenterology center. She said that her office had received a referral from Dr. Issac. She wanted to schedule an appointment for Dad to have his G-tube changed and to discuss
Later in the morning, I received a call from Barbara at the Scott & White gastroenterology center. She said that her office had received a referral from Dr. Issac. She wanted to schedule an appointment for Dad to have his G-tube changed and to discuss  Shortly before I was ready to log off for the day, Dad wanted to make his way into the office, which was no easy task. Although the door was wide enough for the wheelchair, the placement of a large desk just inside the door made wheelchair access impossible. Gale and I had to carefully transfer him from the stable wheelchair to the less stable
Shortly before I was ready to log off for the day, Dad wanted to make his way into the office, which was no easy task. Although the door was wide enough for the wheelchair, the placement of a large desk just inside the door made wheelchair access impossible. Gale and I had to carefully transfer him from the stable wheelchair to the less stable  I had assumed that Michell would replace Gale tomorrow, but I hadn’t heard anything from Becky, the owner of One on One Personal Home Care. I dashed off a quick email to her to confirm, and then returned to my day job.
I had assumed that Michell would replace Gale tomorrow, but I hadn’t heard anything from Becky, the owner of One on One Personal Home Care. I dashed off a quick email to her to confirm, and then returned to my day job. Dad was still very tired and was ready for bed shortly after Mom was declared the Oh Hell winner of the night. By 7:30 P.M., he was in bed and ready for me to administer his meds and trach care. I sat with him while Gale prepared herself for bed, and then went upstairs to call Stan. To say the least, my updates to him about the daily events were varied from day to day. Because Dad went to bed early, I was also able to retire early and hoped to get an extra 30 minutes of sleep.
Dad was still very tired and was ready for bed shortly after Mom was declared the Oh Hell winner of the night. By 7:30 P.M., he was in bed and ready for me to administer his meds and trach care. I sat with him while Gale prepared herself for bed, and then went upstairs to call Stan. To say the least, my updates to him about the daily events were varied from day to day. Because Dad went to bed early, I was also able to retire early and hoped to get an extra 30 minutes of sleep. Michell arrived at 11:00 A.M. and conferred with Gale for a few minutes. It was nice to have a few weeks in a row with the same two aides. The transitions were easier for them and they were getting to know one another. Shortly after Gale left, Dad wanted to lie down for a short nap.
Michell arrived at 11:00 A.M. and conferred with Gale for a few minutes. It was nice to have a few weeks in a row with the same two aides. The transitions were easier for them and they were getting to know one another. Shortly after Gale left, Dad wanted to lie down for a short nap. Dad and Michell were sound asleep when I woke them shortly after 4:00 A.M. We had an uneventful morning and Dad was picked up for dialysis shortly before 6:00 A.M. His dialysis session was finished before 11:00 A.M., and they were home before noon. After administering his midday meds and trach care, he was ready for a nap.
Dad and Michell were sound asleep when I woke them shortly after 4:00 A.M. We had an uneventful morning and Dad was picked up for dialysis shortly before 6:00 A.M. His dialysis session was finished before 11:00 A.M., and they were home before noon. After administering his midday meds and trach care, he was ready for a nap. After dinner, Dad felt well enough to play a couple of games of Oh Hell: Dad won the first game and Mom won the second. We had two sets of criteria that determined how long we played cards: how Dad felt and whether he had dialysis the next day and how I felt and whether I had to work the next day. For the most part, I wanted to start Dad’s nighttime routine by 8:30 P.M. so that I could go to sleep by 9:30 P.M. A perfect night was one in which we all got six hours of uninterrupted sleep.
After dinner, Dad felt well enough to play a couple of games of Oh Hell: Dad won the first game and Mom won the second. We had two sets of criteria that determined how long we played cards: how Dad felt and whether he had dialysis the next day and how I felt and whether I had to work the next day. For the most part, I wanted to start Dad’s nighttime routine by 8:30 P.M. so that I could go to sleep by 9:30 P.M. A perfect night was one in which we all got six hours of uninterrupted sleep.
 commode that we kept in the common area of the bathroom. Having it in a more open area enabled the aides to transport him to and from the commode, a contraption that he loathed. After helping him into the bathroom to use the dreaded bedside commode, Gale and I were able to convince him to go back to bed. Thankfully, he remained in bed until 8:30 A.M., at which time I administered his trach care and morning meds. I was still a rookie with the trach care and the process took about 45 minutes.
commode that we kept in the common area of the bathroom. Having it in a more open area enabled the aides to transport him to and from the commode, a contraption that he loathed. After helping him into the bathroom to use the dreaded bedside commode, Gale and I were able to convince him to go back to bed. Thankfully, he remained in bed until 8:30 A.M., at which time I administered his trach care and morning meds. I was still a rookie with the trach care and the process took about 45 minutes. also needed to bring a blanket, a box of tissues, and various other items. Gale told Stan that instead of Mom’s Elizabeth Arden tote bag that we were using to transport his dialysis accessories, Dad needed something larger and more masculine, like a duffle bag. Stan wasn’t sure what she had in mind, but he eventually found a gym bag that she deemed perfect for the task.
also needed to bring a blanket, a box of tissues, and various other items. Gale told Stan that instead of Mom’s Elizabeth Arden tote bag that we were using to transport his dialysis accessories, Dad needed something larger and more masculine, like a duffle bag. Stan wasn’t sure what she had in mind, but he eventually found a gym bag that she deemed perfect for the task. During dialysis, Dad used oxygen tanks from the dialysis center, but this service did not include the moisture that he needed to keep his trach moist. In an attempt to compensate for the lack of moisture, Timothy from American HomePatient had provided us with several bibs composed of a porous non-woven material. The bib was placed between the trach and the oxygen source. The bib wouldn’t stay moist for more than 30 minutes, so we kept a small spray bottle in his dialysis bag, and Gale was vigilant about keeping the bib wet.
During dialysis, Dad used oxygen tanks from the dialysis center, but this service did not include the moisture that he needed to keep his trach moist. In an attempt to compensate for the lack of moisture, Timothy from American HomePatient had provided us with several bibs composed of a porous non-woven material. The bib was placed between the trach and the oxygen source. The bib wouldn’t stay moist for more than 30 minutes, so we kept a small spray bottle in his dialysis bag, and Gale was vigilant about keeping the bib wet.
 Addison, one of the
Addison, one of the  When the three of us arrived at the house, Mom told us that last night she had washed her slippers and had left them on the bench in the courtyard.When she woke up today, only one slipper remained. The neighbors share stories of the wildlife in the area. I decided to try my luck slipper hunting in the backyard. Sure enough, I found it under a tree, none the worse for wear. Something that seemed like a tasty treat must have left its predator with a little dry mouth. Dad would love this story.
When the three of us arrived at the house, Mom told us that last night she had washed her slippers and had left them on the bench in the courtyard.When she woke up today, only one slipper remained. The neighbors share stories of the wildlife in the area. I decided to try my luck slipper hunting in the backyard. Sure enough, I found it under a tree, none the worse for wear. Something that seemed like a tasty treat must have left its predator with a little dry mouth. Dad would love this story. Wednesday, July 22, 2015: 3:45 P.M. I had just left a meeting at work and listened to the voicemail that my mother left 40 minutes earlier. “Melody, it’s Mom. I’m at the hospital with Dad and he’s not doing too well. He had a bad coughing spell during dialysis and they’re trying to bring his blood pressure down, but he’s got the shakes and delusions and all kinds of stuff. Call me on my cell, because I’m not going to leave him. Talk to you later. Bye-bye.”
Wednesday, July 22, 2015: 3:45 P.M. I had just left a meeting at work and listened to the voicemail that my mother left 40 minutes earlier. “Melody, it’s Mom. I’m at the hospital with Dad and he’s not doing too well. He had a bad coughing spell during dialysis and they’re trying to bring his blood pressure down, but he’s got the shakes and delusions and all kinds of stuff. Call me on my cell, because I’m not going to leave him. Talk to you later. Bye-bye.”