October 2. It was 2:00 A.M., and Dad was wide awake and wanted to get up. After Gale, our caregiver, called me for assistance, she resituated Dad in bed and helped him roll over on his side, although she noticed he didn’t need her assistance. To keep him on his side and more or less stuck in bed, she wedged a pillow behind him. I don’t know if he slept, but at 4:00 A.M., Gale paged me again when Dad tried to get out of bed, so the pillow didn’t do much to control him.
My parents’ bathroom was large, but the commode was located in a separate room, which was more like a closet. In his current condition, it was physically impossible for him to use the commode. American HomePatient (AHP) provided us with a bedside  commode that we kept in the common area of the bathroom. Having it in a more open area enabled the aides to transport him to and from the commode, a contraption that he loathed. After helping him into the bathroom to use the dreaded bedside commode, Gale and I were able to convince him to go back to bed. Thankfully, he remained in bed until 8:30 A.M., at which time I administered his trach care and morning meds. I was still a rookie with the trach care and the process took about 45 minutes.
commode that we kept in the common area of the bathroom. Having it in a more open area enabled the aides to transport him to and from the commode, a contraption that he loathed. After helping him into the bathroom to use the dreaded bedside commode, Gale and I were able to convince him to go back to bed. Thankfully, he remained in bed until 8:30 A.M., at which time I administered his trach care and morning meds. I was still a rookie with the trach care and the process took about 45 minutes.
I received a call from Kathleen Devine (I loved her name.), who introduced herself as the home care physical therapist. She wanted to stop by to assess Dad’s strength to determine a plan for his occupational and physical therapies. Our schedule was wide open and she said that she would stop by before noon.
After a couple of trips to dialysis, we had realized that in addition to his extra trach, Dad  also needed to bring a blanket, a box of tissues, and various other items. Gale told Stan that instead of Mom’s Elizabeth Arden tote bag that we were using to transport his dialysis accessories, Dad needed something larger and more masculine, like a duffle bag. Stan wasn’t sure what she had in mind, but he eventually found a gym bag that she deemed perfect for the task.
also needed to bring a blanket, a box of tissues, and various other items. Gale told Stan that instead of Mom’s Elizabeth Arden tote bag that we were using to transport his dialysis accessories, Dad needed something larger and more masculine, like a duffle bag. Stan wasn’t sure what she had in mind, but he eventually found a gym bag that she deemed perfect for the task.
Gale checked out Dad’s bureau and closet. She marveled at how well his clothes were folded and organized, although I don’t know if the credit goes to Dad or Mom. With a little guidance from Dad, Gale picked out some clothes for him and dressed him for the day. Gale also made a slight design adjustment to Dad’s undershirt. Because his PEG tube extended out from his midsection, wearing an undershirt over the tube bent the tube, which, in addition to being uncomfortable, was not good for the PEG tube. With Dad’s permission and the precision of Edward Scissorhands, Gale cut a hole in his undershirt and fished the tube through the opening. When Dad wore a button-down shirt, the tube extended through the placket. The PEG tube wardrobe problem was solved.
By 9:30 A.M., Gale and I had transferred Dad to the wheelchair and Gale wheeled him outside on the porch. Dad could navigate the wheelchair pretty well by himself in the house, but he needed some assistance going through the thresholds to the outside. By 10:00 A.M., I insisted that he come back inside so that we could hook him up to the moist air. He wasn’t enamored with the thought of being tethered to the concentrator and nebulizer, but after Mom brought him the paper he seemed pretty satisfied to sit in his room to read it. He hadn’t read a newspaper since July.
At 11:45 A.M., Kathleen arrived. She was a no-nonsense transplant from New York and I liked her immediately. She watched as Gale and I transferred Dad from the wheelchair to the bed and back again. She told us that a physical therapist aide would stop by twice a week to help him stand and walk, and the occupational therapist would visit him once a week and work on his upper body and core strength. We agreed that Dad would have physical therapy on Monday and Wednesday and occupational therapy on Friday. When I asked about speech therapy to address his swallowing problems, she said that I would have to speak with Adan about swallow therapy.
A few minutes after Kathleen left, the doorbell rang again, and this time it was Paula, the home care nurse. According to the plan that we had established during Dad’s admission to home care, the home care nurse would visit us three times a week. Although I was glad to have the nurses stop by, I was also nervous that they would find fault with something that we were or were not doing. Paula told us that Dad’s bed sore, which started when he fell in May, was serious, and she suggested that we get some Mepilex border patches. She had a couple of extras in her bag but told us that they were expensive and that we should ask AHP to supply them for us.
When Paula left, I called AHP but was told that without a doctor’s order, Medicare would not reimburse them. To obtain doctor’s orders would require that I contact Dad’s primary care physician and schedule an appointment, and this activity was not high on my list of priorities, so I decided to buy a package myself. Also, when Gale and I snagged supplies from Dad’s room at the CCH, I grabbed a box of gloves, size small, which were fine for me but were too small for Gale. I logged on to Amazon.com and ordered the Mepilex patches and a case of medium gloves. Was there anything that this company didn’t sell?
After his busy day of visitors, and a tremendous lack of sleep, Dad finally let us put him back in bed and he slept for two glorious hours.
Shortly before 5:00 P.M., Dad wanted to get out of bed and visit with us while we partook of some alcoholic beverages. Happy hour at the Locke house had been a nightly ritual that he could now only watch. Before the surgery last May, my Dad’s Manhattans had been a highlight of the overnight visit to my parents’ house that my girlfriends looked forward to every year.
At 7:30 P.M., we began what was becoming our nightly ritual. I administered the trach care and the meds, and Gale changed out the tube feed bag and filled the new one with Nepro. Gale was quickly becoming a pro at winding the tubing through the Kangaroo pump, and I knew that I needed to start paying more attention to what she was doing. It was unfortunate that the bag did not hold enough Nepro to make it through the night. Fortunately, I guess, Dad didn’t sleep through the night anyway.
October 3. At 2:20 A.M., Gale woke to find that Dad was halfway out of the bed, which prompted her to use the baby monitor to page me. Gale and I maneuvered him back into bed, but he insisted that he was going to get up. I told him that if he didn’t stay in bed, I would get into the bed next to him so that he couldn’t escape. He said, “OK,” and scooted over. Two hours later, we were up and I had a dandy kink in my neck from sleeping halfway off of the pillow. Gale and I transferred Dad to the wheelchair and he wheeled himself to the sink in the bathroom, where he washed his face and brushed his teeth. As he held his hands and washcloth under the faucet, he said that this was the first time in five months that he had felt running water on his hands. Gale and I exchanged glances, too overcome to say anything in response. He neglected to mention that it had also been five months since he had brushed his teeth and washed his face. These milestones helped to put Dad in a great mood.
I administered his morning meds and trach care and Gale dressed him for dialysis. He was ready for the ambulance transport at 6:10 A.M., 10 minutes before his scheduled pickup time. Dad’s great mood diminished somewhat when the transport arrived at 7:20 A.M., 20 minutes after his session was supposed to start. He was eventually hooked up at 8:00 A.M.
 During dialysis, Dad used oxygen tanks from the dialysis center, but this service did not include the moisture that he needed to keep his trach moist. In an attempt to compensate for the lack of moisture, Timothy from American HomePatient had provided us with several bibs composed of a porous non-woven material. The bib was placed between the trach and the oxygen source. The bib wouldn’t stay moist for more than 30 minutes, so we kept a small spray bottle in his dialysis bag, and Gale was vigilant about keeping the bib wet.
During dialysis, Dad used oxygen tanks from the dialysis center, but this service did not include the moisture that he needed to keep his trach moist. In an attempt to compensate for the lack of moisture, Timothy from American HomePatient had provided us with several bibs composed of a porous non-woven material. The bib was placed between the trach and the oxygen source. The bib wouldn’t stay moist for more than 30 minutes, so we kept a small spray bottle in his dialysis bag, and Gale was vigilant about keeping the bib wet.
Dad stayed alert during the entire dialysis session, and he and Gale talked the entire time. I imagine that Gale would have appreciated his taking a little nap so that she could close her eyes. Dad’s blood pressure had dropped somewhat during dialysis, so the dialysis nurse stopped the session before the goal of 1500 ml was reached. Gale called the EMT service for a ride, and once again they waited for more than an hour for a ride home. We were starting to set some pretty low expectations for the EMT transport service.
After they returned home, Dad was tired and wanted to take a nap. During the two hours that he slept, Gale also slept. At 4:00 P.M., Dad was awake and ready to get up. Gale and I transferred him to his wheelchair and we went outside and sat on the patio for 90 minutes. He had been away from the nebulizer for almost six hours today, so I strongly suggested that he go back to his room. My husband, Stan, was still in town, and he visited with Dad until 7:00 P.M., when Mom served dinner. In addition to the baby monitor station in my bedroom, we also kept one of the stations in the dining room. Just a few minutes into dinner, we heard an unusual sound from the monitor. Gale practically leapt from her chair and ran to the bedroom and found my father on the floor on the right side of his bed. In addition to the oxygen, he was also receiving nutrition from the tube feed. All of this equipment was located on the left side of the bed, which meant that he was putting a strain on a couple of vital supplies by being on the floor. It astonished me that he couldn’t figure out that in addition to being too weak to stand, he was also tethered. Fortunately, Stan was there and he, Gale, and I got Dad up off the floor and into the wheelchair. Gale checked his PEG and looked for skin tears and I checked his trach. He hadn’t hurt himself, but he gave the rest of us a scare.
Gale stayed with Dad while Mom, Stan, and I finished dinner. I then sat with him while Gale ate. When she was finished, Gale started getting Dad ready for bed. After he was dressed for bed, Gale and I ran through our nightly routine of meds, trach care, and tube feed.
Starting at 10:00 P.M., he started trying to get out of bed. He might have been too weak to stand, but Gale thought that for a weak guy, he was pretty strong. He could really put up a battle when he wanted to get out of bed.
October 4. The baby monitor alarm woke me at 4:00 A.M. Gale thought that Dad sounded gurgly and thought that he might need to be suctioned. I agreed and after I finished suctioning him, he insisted that he wanted to use the house toilet. Gale and I tried to explain that he couldn’t use it but that we would take him to the bedside commode in the bathroom. To say the least, he became very upset. He complained that the commode seat was very uncomfortable, which was true. He finally relented, but then he didn’t want to go back to bed, so Gale got him up and prepared for the day. I promised Dad that I would order a seat cushion for him, which I did later in the day.
By 6:00 A.M., he was sitting in the wheelchair, attached to the moist oxygen, and reading the paper, and we were all happy.
After breakfast, I returned to Dad’s room and administered his morning meds and trach care and then excused myself to shower and get ready for church. At 10:20 A.M., my mother and I escaped to church. Our friends at church were anxious to hear about Dad. Sue, our friend who was the nurse practitioner at the dialysis center, said that Dad was a real chatterbox. She had been amazed by how much he talked during dialysis. The pastors and everyone else we told about Dad were thrilled that he was at home.
Shortly before we returned home from church around 12:30 P.M., Dad felt a little tired and wanted to go back to bed to rest. Gale mentioned to me that she had heard some noise coming from his stomach and told me that she was going to ask the nurse to listen more closely tomorrow.
My husband had been staying with us for the past week, but after lunch, he went back home to Houston. I don’t know how we would have managed without him and I hoped that we wouldn’t need his brawn while he was gone. For both of us, our vacation had now come to an end. I had set up my work computer in my parents’ office and planned to start back to work tomorrow at 4:30 A.M.
Tonight was another frustrating night of Dad trying to get out of bed. We had him ready for bed at 8:30 P.M., but he slept until 11:00 P.M., after which time he tried repeatedly to get out of bed. At 2:00 A.M., Gale used the baby monitor alarm to call me. Dad had scooted to the end of the bed and she needed help to raise him. He insisted that he wanted to get up. I explained to him that I had to go back to work in a couple of hours and that I wanted him to sleep until 4:00 A.M., which was when I would get up. He agreed to that plan, and the three of us slept for two more hours. I fantasized about six consecutive hours of sleep.



 September 12. Mom and I arrived at the CCH at 8:00 A.M. Dad was still restrained and his call button was on the floor. John, Dad’s nurse, told us that his heart rate had been elevated to 135 and he became
September 12. Mom and I arrived at the CCH at 8:00 A.M. Dad was still restrained and his call button was on the floor. John, Dad’s nurse, told us that his heart rate had been elevated to 135 and he became 


 August 9, 2015. We arrived at the hospital at 9:00 A.M. to find that Dad was still asleep and restrained, the nurse’s name was not on the board, and Dad’s feeding tube was empty. Two out of three of these situations were unacceptable. I went to the nurse’s station to find out who his nurse was and to let them know that his tube feed bottle was empty. A nurse entered the room with a fresh bottle of Nepro, changed out his tubing, and replaced the empty bottle. The nurse also told me that Dad’s nurse was Nicole, who finally showed up at 9:15 A.M. and introduced herself.
August 9, 2015. We arrived at the hospital at 9:00 A.M. to find that Dad was still asleep and restrained, the nurse’s name was not on the board, and Dad’s feeding tube was empty. Two out of three of these situations were unacceptable. I went to the nurse’s station to find out who his nurse was and to let them know that his tube feed bottle was empty. A nurse entered the room with a fresh bottle of Nepro, changed out his tubing, and replaced the empty bottle. The nurse also told me that Dad’s nurse was Nicole, who finally showed up at 9:15 A.M. and introduced herself. August 10. We arrived at 7:40 A.M. and noticed that Dad was already on dialysis. Before we arrived, they had drawn blood and ran an
August 10. We arrived at 7:40 A.M. and noticed that Dad was already on dialysis. Before we arrived, they had drawn blood and ran an 

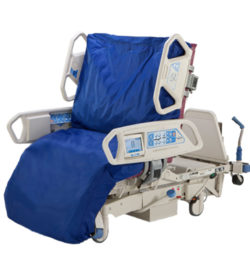 August 3, 2015. It had now been 90 days since Dad first entered the hospital for his seven-to-ten day stay. When Mom and I arrived at 7:45 A.M., Dad’s room was a hubbub of activity. Dr. Phan, the nephrology resident, was assessing him and Emily, his nurse, was exercising his arms and legs. But the first thing that we noticed was Dad’s bed. Yesterday, Dr. Jimenez had told Dad’s nurse that he wanted to see Dad’s bed raised to a more upright position. I had envisioned that the angle of his bed would change from 30 to 75 degrees. What we saw instead was a bed that had morphed into a chair. It played music, automatically adjusted to specific angles, and could change into a chair. Was there anything that this bed couldn’t do?
August 3, 2015. It had now been 90 days since Dad first entered the hospital for his seven-to-ten day stay. When Mom and I arrived at 7:45 A.M., Dad’s room was a hubbub of activity. Dr. Phan, the nephrology resident, was assessing him and Emily, his nurse, was exercising his arms and legs. But the first thing that we noticed was Dad’s bed. Yesterday, Dr. Jimenez had told Dad’s nurse that he wanted to see Dad’s bed raised to a more upright position. I had envisioned that the angle of his bed would change from 30 to 75 degrees. What we saw instead was a bed that had morphed into a chair. It played music, automatically adjusted to specific angles, and could change into a chair. Was there anything that this bed couldn’t do? While Mom and I were at home for dinner, I printed out some recent photos of Dad with the family. I wanted the hospital personnel to see him as more than the sick man that they attended in that hospital bed. He hadn’t entered the hospital as some sickly old man, and I wanted them to have a sense of who he was just a few months earlier. After dinner, Mom and I returned to the hospital around 6:50 P.M. and learned that Dustin was Dad’s nurse. I wasn’t impressed with this nurse, and I wasn’t thrilled to see him again.
While Mom and I were at home for dinner, I printed out some recent photos of Dad with the family. I wanted the hospital personnel to see him as more than the sick man that they attended in that hospital bed. He hadn’t entered the hospital as some sickly old man, and I wanted them to have a sense of who he was just a few months earlier. After dinner, Mom and I returned to the hospital around 6:50 P.M. and learned that Dustin was Dad’s nurse. I wasn’t impressed with this nurse, and I wasn’t thrilled to see him again. Carlos, the dialysis nurse, arrived at 8:15 A.M. and proceeded to prepare Dad for dialysis. At the same time, Dr. Fernandez, one of the
Carlos, the dialysis nurse, arrived at 8:15 A.M. and proceeded to prepare Dad for dialysis. At the same time, Dr. Fernandez, one of the  At 2:15 P.M., the hematology team arrived. Because Dad’s lab work showed that he had
At 2:15 P.M., the hematology team arrived. Because Dad’s lab work showed that he had  Dad’s oxygen levels had been fair, and when Nikita, the respiratory therapist arrived, she increased his oxygen level on the ventilator from 40% to 50%. As she adjusted the ventilator settings, she said that she’d probably decrease the levels back to 40% later in the day.
Dad’s oxygen levels had been fair, and when Nikita, the respiratory therapist arrived, she increased his oxygen level on the ventilator from 40% to 50%. As she adjusted the ventilator settings, she said that she’d probably decrease the levels back to 40% later in the day. Jennifer from PT arrived and Dad was ready to exercise. He immediately asked about her plans for him, and Mom wanted to know what he could do over the weekend. She didn’t want him “just lying in bed.” Although my parents were resigned to the fact that my father had to remain hospitalized until August 26, they didn’t want to stay there one day longer than absolutely necessary. Jennifer showed them a variety of exercises that Dad could do, and she encouraged him to sit in the chair at least twice a day over the weekend. Although he started out pretty unsteady, Dad was able to walk with assistance for about 250 feet. Jennifer was encouraged about how his mobility kept improving during their sessions.
Jennifer from PT arrived and Dad was ready to exercise. He immediately asked about her plans for him, and Mom wanted to know what he could do over the weekend. She didn’t want him “just lying in bed.” Although my parents were resigned to the fact that my father had to remain hospitalized until August 26, they didn’t want to stay there one day longer than absolutely necessary. Jennifer showed them a variety of exercises that Dad could do, and she encouraged him to sit in the chair at least twice a day over the weekend. Although he started out pretty unsteady, Dad was able to walk with assistance for about 250 feet. Jennifer was encouraged about how his mobility kept improving during their sessions. The nurse started a new IV, but they had no plans to remove Dad’s
The nurse started a new IV, but they had no plans to remove Dad’s 
 For the past few weeks, Mom and I had been unable to unlock the front door with the house key. Stan had sprayed graphite into the lock and that remedy had worked for a couple of weeks, but we were now back to square one. We didn’t have the time or inclination to fix it, so we just accessed the house from other doors. The front door lock was just an example of life’s little inconveniences that didn’t seem all that important at the time.
For the past few weeks, Mom and I had been unable to unlock the front door with the house key. Stan had sprayed graphite into the lock and that remedy had worked for a couple of weeks, but we were now back to square one. We didn’t have the time or inclination to fix it, so we just accessed the house from other doors. The front door lock was just an example of life’s little inconveniences that didn’t seem all that important at the time. July 15. During dialysis, Dad told the nephrologist that he wanted to go home. The doctor told him that to be declared dialysis dependent (with End Stage Renal Disease), he had to be hospitalized and on dialysis for a total of 12 weeks. Although Mom and I had heard this news a few days ago, it was new news for Dad and prompted him to start asking questions about billing. The doctor contacted Marty Edens, the social worker, who dropped by to answer his questions. Marty couldn’t answer his specific billing questions, but she was familiar with Medicare and some of Dad’s situation. Dad told Marty that he “can’t imagine being here for six more weeks.” He repeatedly told her that he “
July 15. During dialysis, Dad told the nephrologist that he wanted to go home. The doctor told him that to be declared dialysis dependent (with End Stage Renal Disease), he had to be hospitalized and on dialysis for a total of 12 weeks. Although Mom and I had heard this news a few days ago, it was new news for Dad and prompted him to start asking questions about billing. The doctor contacted Marty Edens, the social worker, who dropped by to answer his questions. Marty couldn’t answer his specific billing questions, but she was familiar with Medicare and some of Dad’s situation. Dad told Marty that he “can’t imagine being here for six more weeks.” He repeatedly told her that he “
 July 9. Dr. Smith said that in terms of his respiratory status, Dad was doing well. Unfortunately, he still had too many secretions to have his trach tube red-capped. He also said that, although it was still elevated, Dad’s creatinine levels seemed to be dropping. He wasn’t going to make any predictions but thought that Dad might be having some recovery of his kidney function. Wouldn’t that be great!
July 9. Dr. Smith said that in terms of his respiratory status, Dad was doing well. Unfortunately, he still had too many secretions to have his trach tube red-capped. He also said that, although it was still elevated, Dad’s creatinine levels seemed to be dropping. He wasn’t going to make any predictions but thought that Dad might be having some recovery of his kidney function. Wouldn’t that be great! Before Mom and I left for the day, Dad told Mom to be sure to give the neighbors some of our cantaloupes. Mom said that she had planned to give them away and would start with our neighbors to the north after we got home.
Before Mom and I left for the day, Dad told Mom to be sure to give the neighbors some of our cantaloupes. Mom said that she had planned to give them away and would start with our neighbors to the north after we got home.