September 1, 2015. Dad was awake at 3:40 A.M. and was convinced that there were animals in his room. Regardless of what Michelle, his nurse, said, he insisted that they were there and he wanted her to move his bed so that he could get a better view of them. Michelle tried her best to reorient him to his surroundings by asking him some questions, but he would answer only a few of them. After he became somewhat oriented, she gave Dad his call light and left his room. A few additional hours of sleep didn’t seem to help Dad, as he still seemed somewhat confused when he woke up later.
When Jennifer arrived for Dad’s physical therapy session, Dad said that he wasn’t feeling very well, but would try to participate. She got him to do some bed exercises and eventually got him to sit on the edge of the bed. From that point on, he refused to participate and said that he wanted to lie down. She was able to assist him into the Stryker cardiac chair and then left him with Mom. Mom took him outside, and he was amazed by it; he had not been outside in almost four months, and he thoroughly enjoyed the different sensory experience.
I was in Houston, but right about that time, I received a text message from Pastor Don, who asked for Mom’s mobile phone number. He must have been near the CCH because he texted me right back that Mom and Dad were outside the building but were heading indoors. Mom had never seen Don’s car before and didn’t realize that he was in the parking lot.
After my parents returned to Dad’s room, Dad wanted to know if he and Mom were going shopping. Given his current circumstances, it was an odd question but was typical of a question he might have asked some five months earlier. While three nurses moved Dad from the Stryker chair back into bed, Pastor Don came inside and the three of them had a nice visit. There was something about visits from male friends that seemed to make Dad more lucid and engaged. We had had a similar experience when our neighbor, Tom, visited.
Dad had been receiving fentanyl for his shoulder pain, and he was sleeping when Mom returned from lunch. Mom had been told that they were reducing his dosage, but he sure seemed sleepy. After he woke up, he and Mom had a nice afternoon. She told him about the rehab facility that she and I had visited and she also told him about rehab therapy that he could receive at home.
September 2. Shortly after midnight, Dad was wide awake and very confused. Konnie, his nurse, tried to reorient him, but Dad could not recall his birth date, the time, the date, or the president. Konnie spent quite a while reorienting Dad, and then Dad slept until he was awakened shortly before 7:00 A.M. for dialysis. However, according to Suzanne, the dialysis nurse, Dad was still pretty disoriented when he arrived for his session.
When Mom arrived, Dad immediately started talking about going home, and he kept on topic for the entire day. He just could not understand why he couldn’t leave and eventually got mad at Mom for not taking him out of this place. The nurses tried to help by giving him some medication to calm his agitation.
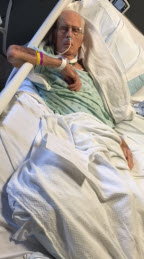 Addison, one of the speech pathologists that we knew from Memorial, arrived to administer another bedside swallow study. The last one, which was administered by Holly, was a total bust. Dr. White had ordered this evaluation at my request a couple of days ago. Unfortunately, Dad responded about as well to Addison as he had to Holly a few days earlier on August 31. He refused to participate and Mom had to read him the riot act to get him to work with Addison. His swallows were delayed for a few seconds and he coughed each time he swallowed. When Addison instructed him to use his Yankauer to suction himself, he flatly refused. She tried to explain the consequences to him, but the effort was wasted breath on her part. A few minutes after Addison completed the evaluation, the respiratory therapist suctioned out the brown and purple fluid that he had aspirated during the test. Because of another failed bedside evaluation, Addison could not recommend him for the modified barium swallow study (MBSS), which would further assess his readiness to have his trach red-capped. Dad’s delirium seemed to be getting worse, and I couldn’t help but wonder what they had given Dad earlier in the day to calm him.
Addison, one of the speech pathologists that we knew from Memorial, arrived to administer another bedside swallow study. The last one, which was administered by Holly, was a total bust. Dr. White had ordered this evaluation at my request a couple of days ago. Unfortunately, Dad responded about as well to Addison as he had to Holly a few days earlier on August 31. He refused to participate and Mom had to read him the riot act to get him to work with Addison. His swallows were delayed for a few seconds and he coughed each time he swallowed. When Addison instructed him to use his Yankauer to suction himself, he flatly refused. She tried to explain the consequences to him, but the effort was wasted breath on her part. A few minutes after Addison completed the evaluation, the respiratory therapist suctioned out the brown and purple fluid that he had aspirated during the test. Because of another failed bedside evaluation, Addison could not recommend him for the modified barium swallow study (MBSS), which would further assess his readiness to have his trach red-capped. Dad’s delirium seemed to be getting worse, and I couldn’t help but wonder what they had given Dad earlier in the day to calm him.
Shortly after 3:30 P.M., Susan stopped by for Dad’s physical therapy session. Dad had been asking all day to get out of bed. That he kept trying to get out of bed to walk to the bathroom was ironic, because he could not stand without some assistance, let alone walk. When Susan finished his session with him, she moved him to the Stryker chair with the air mattress. She admitted that Dad was making progress, albeit, very slowly.
Mom had been a little disappointed about the day. Dad had made little or no progress toward the goals laid out for him by the doctor, and Dad’s time with hospitalization coverage was quickly slipping away.
September 3. If only Dad could sleep through the night. Once again, he was awake in the middle of the night, and he set off the bed alarm when he attempted to get out of bed. He told the nurse that he needed to get out of bed so that he could go to his office and work on his finances. Konnie, the nurse, tried to reorient Dad to the fact that he was at the CCH and not at home. Dad became verbally aggressive with him and started hitting and kicking Konnie and the nurses who came to the room to assist him. Konnie finally administered Haldol, although Dad still remained pretty combative for a while afterward. His lungs were full of secretions and he needed to be suctioned, but Dad refused to let the respiratory therapist suction him. Finally, the nurse contacted the doctor, who ordered the nurses to restrain him.
When Dr. Anderson arrived later than morning, he decided to address Dad’s delirium by doubling Dad’s bedtime dosage of Seroquel. I had to assume that the increased dosage would decrease his need for restraints. The doctor had ordered that they remain in place because Dad was pulling at his devices earlier in the morning.
Dad had a much better physical therapy session today with Susan. In addition to executing the exercises, she had him use the walker to navigate from the bed to the chair. When she had finished her session with him, she left him in the Stryker chair. After Dad was situated in the chair, Esther put on his restraints.
Mom arrived as Dad was getting into the chair at the end of his physical therapy session with Susan. After the past few days, during which Dad was too weak to complete some of his exercises, Mom was thrilled to see his progress this morning.
Mom approached Dr. Anderson about letting Dad have some ice. Dad had been allowed to have some ice chips a few times each day when he was at Memorial. Holly and Addison, the speech therapists at Memorial, had told us that even if he aspirated a little of the water from the ice, it would be absorbed by his lungs. Mom thought that if he had some ice chips a few times each day, he would get some practice swallowing. The doctor said that there wasn’t any point in letting Dad have any ice because he would never learn how to swallow. Dr. Anderson added that it was “pointless [to give him ice] because Dad had aspirated so many times” since he left Memorial. Before he left the room, Mom told the doctor that she was going to check out the local dialysis center. In his typical encouraging manner, Dr. Anderson said that she’d “have to go a long way to find a dialysis center that would accept him.”
Mom had made an appointment with the director of the Scott & White dialysis center. Mom later told me that the meeting went well and that she left the meeting with the impression that the trach would not prevent Dad from receiving dialysis there.
Shortly after Mom left for her appointment with the director of the dialysis center, Dad asked Esther, his nurse, why he was restrained. She reminded him about his aggressive behavior during the night. When Dad asked to have the restraints removed, Esther told him about the requirements for removing them. He said that he understood and indicated that he would be more cooperative.
A few minutes after his restraints were removed, Dr. Sangeetha Ranganath, the infectious diseases specialist, stopped by for another assessment. Dr. Ranganath was a sweet Indian woman, but she spoke rapidly with a soft voice and an accent that Mom couldn’t understand. Mom later learned that Dr. Ranganath said that they were keeping him on the same antibiotic for another few weeks.
Dad spent about six hours in the chair and Mom felt like he had had a pretty good day and had made some progress. For her, the day was a mixture of potentially good and discouraging news. Her encounter with Dr. Anderson further hardened her negative feelings toward this doctor. However, she had come away from her meeting with the director of the dialysis center with the impression that they would be able to accommodate Dad.
Konnie was Dad’s night nurse again, and once again, he had difficulty getting Dad to understand that he had to remain in bed. Konnie was only partially successful in reorienting Dad to his situation and had to apply the restraints. He checked on Dad a few times during the night and it seemed like Dad stayed asleep.
September 4. For Dad, one day sort of morphed into the next. For him, today was dialysis day, but for the rest of us, it was the start of the Labor Day weekend. When Dad was wheeled into the dialysis center, he was still wearing his bed restraints. Dad kept attempting to get out of his bed, and Leon, the dialysis nurse, thought that Dad was very confused and disoriented.
While Dad was in dialysis, Mom met with Adan, formerly a speech pathologist at the CCH. She and I had been told by several physicians that Dad should have his feeding tube replaced with the PEG. Unfortunately, we had come to the point where we really didn’t trust some of the attending physicians. She trusted Adan and felt like she could go to him for advice. At the conclusion of their meeting, Mom was ready to tell Dr. Anderson that we wanted to proceed with the PEG procedure.
When she eventually saw the doctor, she told him of her decision. He said that he would order the procedure, but Dad might not get the PEG until Tuesday, the day after Labor Day.
One of Mom’s good friends, Sally, had admitted herself into a SNiF after hip surgery. Mom called her to get a first-hand account of her experience and what we might expect with Dad. With the exception of the food, she said that her experience was positive. She also mentioned that SNiF residents could get a pass to go home on the weekend. This was a benefit that we hadn’t considered.
During the afternoon, Jennifer stopped by for Dad’s physical therapy session. He was very uncooperative and was fixated on scissors and a hair appointment that he supposedly was late for. Jennifer was able to get him to perform only a few range-of-motion exercises during their session.
After work, Stan and I drove to Temple for the long weekend. After dinner, Mom, Stan, and I visited Dad at the CCH. We had the nurse move Dad into the Stryker chair, and then we wheeled him outside and visited with him for about 45 minutes. At 7:45 P.M., we returned Dad to his room, and the three of us returned to the house.
After we left, Dad was moved back into the bed, where the nurse reapplied his restraints.
 When the three of us arrived at the house, Mom told us that last night she had washed her slippers and had left them on the bench in the courtyard.When she woke up today, only one slipper remained. The neighbors share stories of the wildlife in the area. I decided to try my luck slipper hunting in the backyard. Sure enough, I found it under a tree, none the worse for wear. Something that seemed like a tasty treat must have left its predator with a little dry mouth. Dad would love this story.
When the three of us arrived at the house, Mom told us that last night she had washed her slippers and had left them on the bench in the courtyard.When she woke up today, only one slipper remained. The neighbors share stories of the wildlife in the area. I decided to try my luck slipper hunting in the backyard. Sure enough, I found it under a tree, none the worse for wear. Something that seemed like a tasty treat must have left its predator with a little dry mouth. Dad would love this story.


2 thoughts on “It’s pointless; he’ll never learn how to swallow”