September 30, 2015. Usually, I woke up with the aid of an alarm—most recently, the alarm on my iPhone. Today marked the start of a new wake-up system: the baby monitor in Dad’s room. The good thing about it was that I could hear everything that happened in his room. The bad thing about the monitor was that I could hear everything that happened in his room. If the beds at Scott & White represented the Mercedes-Benz of hospital beds, Dad’s new bed was more like a beat-up jalopy. Not only was it operated with hand cranks, it squeaked whenever Dad moved, which I could hear clearly through the monitor. With the squeaking bed, the intermittent sound of the suctioning machine, and the constant drone of the oxygen concentrator (oxygen generator), a constant cacophony of sounds emanated from the monitor. Gale had it worse, though. In addition to the noise, the oxygen concentrator and its nebulizer pumped out a lot of heat. Whenever she opened the windows to let in some cooler air, my now skinny and cold-natured father complained about being too cold. This room was the warmest and noisiest room in the neighborhood.
oxygen concentrator (oxygen generator), a constant cacophony of sounds emanated from the monitor. Gale had it worse, though. In addition to the noise, the oxygen concentrator and its nebulizer pumped out a lot of heat. Whenever she opened the windows to let in some cooler air, my now skinny and cold-natured father complained about being too cold. This room was the warmest and noisiest room in the neighborhood.
During Dad’s first day home, Gale and I struggled to establish a routine. I tried to create a schedule in Outlook, but his seemingly-regular schedule wasn’t regular enough to commit it to a calendar. Dad kept Gale and Mom busy with cleaning and laundry, while I kept a nervous eye on his respiratory needs. I felt tentative at best when it came to trach care and asked Gale to stand by during all of my trach care activities.
In addition to the equipment, American HomePatient (AHP) had delivered dozens of boxes of supplies, including trach care and trach changing kits, Nepro tube feed, tube feed bags, tubing, 4×4 gauze pads, and 4×4 splits. We had boxes stacked in the front entry, the garage, the laundry room, and the bedroom. We had tried to organize some of the supplies last night during the chaos of Dad’s homecoming activities, but I needed to take an inventory. I located a carton that contained trach changing kits but found them to be disappointing. I had hoped that I would have something similar to what the hospital used. Not only did each kit lack some of the accessories included with the hospital kits, the suction tube had a much smaller diameter. The tubing also lacked markers that were important in gauging how deep to extend the tubing down Dad’s trach. I tried using one of the kits and couldn’t suction any of Dad’s secretions. I tossed out the tubing and opened one of the kits that Angela, the respiratory therapist, had provided us yesterday.
 I had just a limited supply of the trach kits from Angela, so I used the information on the packaging to search online for a provider. I found the kits at a company called Healthcare Supply Pros, and ordered two cases, each case containing 36 kits. The order set me back $130.00, but these kits would appreciably lower my aggravation and stress levels, so I felt that the expense was worth it. I just hoped that my order would arrive before I ran through my supply of appropriate kits. It was a shame that we had six cases of the trach care kits from AHP.
I had just a limited supply of the trach kits from Angela, so I used the information on the packaging to search online for a provider. I found the kits at a company called Healthcare Supply Pros, and ordered two cases, each case containing 36 kits. The order set me back $130.00, but these kits would appreciably lower my aggravation and stress levels, so I felt that the expense was worth it. I just hoped that my order would arrive before I ran through my supply of appropriate kits. It was a shame that we had six cases of the trach care kits from AHP.
In addition to his meds, Dad needed the protein supplement, Beneprotein. I had only the few packages that we took from the hospital yesterday. After I ordered the trach care kits, I logged on to Amazon.com and ordered a case of it, which would last 25 days.
While I inventoried supplies and created spreadsheets of medications and schedules, Gale inventoried Dad’s skin tears, and found five of them scattered over his body.
Gale took frequent readings of Dad’s oxygen levels, pulse rate, and blood pressure. Early in the afternoon, his blood pressure reading seemed very low. I’m terrible at interpreting blood pressure readings, but while Dad was in the hospital, I became familiar with the mean arterial pressure (MAP), which the 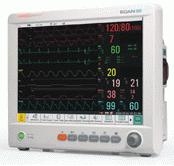 monitors used to trigger alarms for dangerous blood pressure readings. To calculate it, you multiply the systolic (top) number by two, add the product to the diastolic (bottom) number, and then divide by three. In the hospital, the monitor triggered a piercing alarm when the number dipped below 65 (or 60 during dialysis). I quickly performed the calculations, and his MAP was 42, which triggered my own internal alarm. We hadn’t been taking care of Dad for 24 hours and I suddenly felt like the failure that the medical experts thought we would be. In a panic, I called the Home Care office, gave them Dad’s blood pressure reading, and was instructed to call 911. The few minutes that it took for the ambulance to arrive seemed like an hour. When the EMTs arrived, they took Dad’s vitals and found them to be normal. They stayed for a few minutes and checked his blood pressure again. They told us that they could transport Dad to the hospital, but said us that if Dad was their relative, they’d keep him at home and call 911 again if we had more problems. We happily accepted their advice and thanked them as they left.
monitors used to trigger alarms for dangerous blood pressure readings. To calculate it, you multiply the systolic (top) number by two, add the product to the diastolic (bottom) number, and then divide by three. In the hospital, the monitor triggered a piercing alarm when the number dipped below 65 (or 60 during dialysis). I quickly performed the calculations, and his MAP was 42, which triggered my own internal alarm. We hadn’t been taking care of Dad for 24 hours and I suddenly felt like the failure that the medical experts thought we would be. In a panic, I called the Home Care office, gave them Dad’s blood pressure reading, and was instructed to call 911. The few minutes that it took for the ambulance to arrive seemed like an hour. When the EMTs arrived, they took Dad’s vitals and found them to be normal. They stayed for a few minutes and checked his blood pressure again. They told us that they could transport Dad to the hospital, but said us that if Dad was their relative, they’d keep him at home and call 911 again if we had more problems. We happily accepted their advice and thanked them as they left.
One thing that hadn’t changed with Dad’s move home: his propensity to slide down the bed. In addition to his sliding out of the bed, when he slid down the bed, he was no longer sitting at a 30-degree angle, which was one of our cardinal rules. Because of his risk of aspiration, whenever his incline fell below 30 degrees, we had to stop his tube feed. Whenever we repositioned him, we stopped the pump, used the draw sheet to pull him up in the bed, and then restarted the pump. He was too weak to reposition himself in the bed.
Getting Dad out of the bed and into the wheelchair was no less important at home than it had been at the CCH. Dad was pretty weak and it took both Gale and me to transfer him from the bed to the chair. When he was in the wheelchair, we kept him in the room connected to the concentrator and moisture. We could use the oxygen tanks if he left the room, but we’d have to tie wet  bibs around his trach to provide some moist air to his trach and lungs. AHP had suggested several other methods to keep his air supply moist when he was away from the nebulizer, but all of their suggestions required removal of the speaking valve, which was a nonstarter. Dad was able to sit in the wheelchair for almost two hours before he wanted to get back into the bed. He took a couple of cat naps and seemed to be resting well for the remainder of our first full day at home.
bibs around his trach to provide some moist air to his trach and lungs. AHP had suggested several other methods to keep his air supply moist when he was away from the nebulizer, but all of their suggestions required removal of the speaking valve, which was a nonstarter. Dad was able to sit in the wheelchair for almost two hours before he wanted to get back into the bed. He took a couple of cat naps and seemed to be resting well for the remainder of our first full day at home.
Mom, Gale, and I ate dinner in a couple of shifts, which made the hostess side of my mother crazy. She wanted all three of us to have a nice hot meal, but we couldn’t leave Dad unattended.
At 7:00 P.M., Gale had Dad dressed for bed and ready for me to suction his trach and administer his nighttime meds. She and I were exhausted and took turns getting ourselves ready for bed. Unfortunately, we were a lot sleepier than Dad, who, for all intents and purposes, stayed awake all night. Gale and I both tried to get some sleep, but Dad was restless and Gale employed the panic alarm on the baby monitor a couple of times to request my assistance, usually to reposition him in the bed and to suction him. More than once she woke to find his legs hanging out of the bottom of the bed.
October 1. After a night of naps, Gale and I were up at 4:00 A.M. to prepare Dad for dialysis. We moved him from the bed to the wheelchair, and Gale got him cleaned up and applied lotion to his dry and fragile skin. With some assistance from Mom, Gale found some clothes for Dad and got him dressed. He had lost so much weight since May that his clothes swallowed him. The ambulance arrived at 6:40 A.M., about 20 minutes late and at the time that he was to arrive at the dialysis center. Gale rode in the ambulance, and I followed them in my car. Fortunately, the dialysis center was less than five miles from my parents’ home, so we weren’t too late.
Dad had a reservation in the A bay at the dialysis center. Mom had visited with a charge nurse about a month earlier, but this was my first visit. I was overwhelmed by the size of this place. From what I could tell, they could dialyze about 200 people during each shift. As the aides and nurses moved Dad from the stretcher to a bed, I spoke with the nurse at the center who had just trained some of their techs to change out a trach. I had been told by the nurse practitioner at the CCH that Dad couldn’t be dialyzed at this facility because he couldn’t change out his trach. I was moved when I learned that they trained their personnel when they learned that Dad would be a patient. While it might have been true that the dialysis center didn’t have any trach patients, they had no problem with training their personnel to come to the aid of one. The nurse was relieved when I told him that Dad always traveled with an extra trach and all the supplies that would be needed to make the process easier for the tech and less painful for Dad. My minutes of experience with trachs made me an expert on the subject, especially when speaking with someone who knew about as much about trach care as me.
Because Dad would be dialyzed from a dialysis catheter, versus a fistula, only an RN could hook him up to the dialysis machine. To increase his blood pressure for the procedure, I had administered a couple of dissolved Midodrine pills in his PEG tube. His blood pressure usually dropped during dialysis, so at 9:00 A.M., Gale would administer another two Midodrine pills, which I had already dissolved in water. After seeing that Dad and Gale were OK, I went home.
Dad was finished with his session at 11:00 A.M., but he and Gale weren’t picked up by the EMTs until 12:15 P.M. We knew that transport services were a low priority for ambulances, but he had now been away from home for almost six hours, and he was still a pretty sick guy. When he and Gale returned home after the 20-minute trip, Dad was pretty weak. It was also past time for his meds and trach care.
After the EMTs navigated him and their stretcher through the house, Gale and I situated Dad back in bed and hoped that he’d sleep for an hour or two. According to Gale, Dad had not slept at all during dialysis and had talked non-stop most of his time there. Our friend, Sue, who was the nurse practitioner at the dialysis center, stopped by to visit with him and was also surprised by his non-stop talking. After being confined for so many months, I guess he was reacting to a sudden sense of freedom.
Becky Crabtree, the owner of One On One Personal Services, told us that she had business in the area this afternoon and that she planned to stop by to meet us.  I-35, the interstate highway that is the primary route between Dallas and Temple, is notorious for bad accidents that shut down the freeway. Becky was a victim of such a shutdown and arrived about three hours late at 7:30 P.M. Following her arrival, Gale and I transferred Dad to his wheelchair and wheeled him out to our patio where the four of us visited with Becky for about 30 minutes.
I-35, the interstate highway that is the primary route between Dallas and Temple, is notorious for bad accidents that shut down the freeway. Becky was a victim of such a shutdown and arrived about three hours late at 7:30 P.M. Following her arrival, Gale and I transferred Dad to his wheelchair and wheeled him out to our patio where the four of us visited with Becky for about 30 minutes.
 At 8:30 P.M., Gale started preparing Dad for bed. After he was in bed, I administered the meds and trach care. While I was busy with Dad, Gale changed out the tube feed bags, which had to be changed every 24 hours. Dad hated to be without his speaking valve, so I broke with one of Angela’s rules and left it in place during the night. If he needed help, we needed to be able to hear him. He complained when I removed the speaking valve during trach care. I knew that I’d never hear the end of it if I removed it overnight.
At 8:30 P.M., Gale started preparing Dad for bed. After he was in bed, I administered the meds and trach care. While I was busy with Dad, Gale changed out the tube feed bags, which had to be changed every 24 hours. Dad hated to be without his speaking valve, so I broke with one of Angela’s rules and left it in place during the night. If he needed help, we needed to be able to hear him. He complained when I removed the speaking valve during trach care. I knew that I’d never hear the end of it if I removed it overnight.
Gale and I were exhausted and it had been a full day for Dad. We hoped that Dad was just as tired and would sleep through the night.

